“We’re looking for patients,” Jodie Storrow tells me as we stroll alongside an extended hall on the third ground of University Hospital Coventry.
We are heading in direction of Ward 31. This is the place the hospital’s respiratory sufferers are handled.
Jodie, the hospital’s medical operation supervisor for built-in care, has a really particular kind of affected person that she desires.
“One with COPD, who is on the upward trajectory and does not need any additional support at home,” she says.
Share your NHS expertise with Sky News
What she means is a affected person with a chest, lung or respiratory situation, who’s getting higher and might be discharged safely with out worrying a few package deal of care.
These are the kind of sufferers that match the profile for the hospital’s “virtual wards”.
The hospital is working at close to capability. There are sufferers ready in its emergency division who’ve been admitted however can not come as much as a ward as a result of there aren’t any beds accessible.
So Jodie should discover sufferers whose care can proceed remotely at residence.
“Hospitals are very busy,” she explains. “There’s no secret. So if we free up beds on our wards then we free up another bed for someone that needs it.”
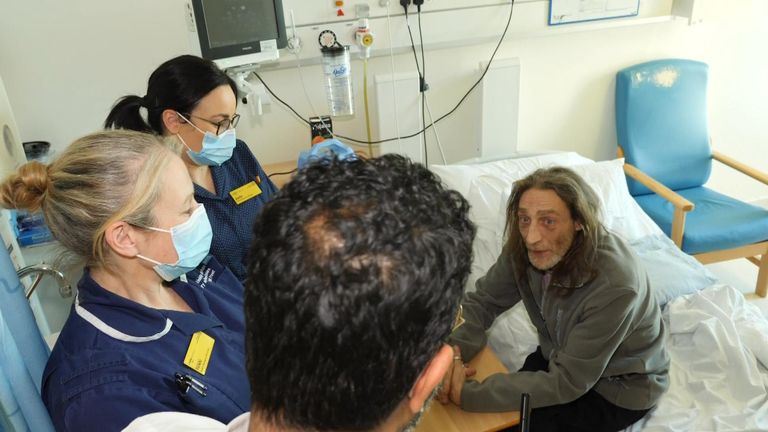
On Ward 31, Jodie finds her affected person, Richard Hall, a retired 56-year-old from Coventry.
Richard was rushed to hospital final week after he nearly fainted after inhaling paint fumes. He has an extended historical past of power lung illness.
Richard has jumped on the probability of being discharged early. He was not anticipating to go residence till subsequent week.
He tells me he’s anxious about staying in hospital and must get again to his flat as rapidly as attainable.
“It’s coming up to Christmas,” he says.
“All my heating and everything is on in my flat as well so I’m burning electricity at the minute. I need to get home and sort things out for Christmas really, so yeah it means everything to me.”
Richard will likely be given a smartphone and requested to take his oxygen and blood stress readings and his temperature as much as 3 times a day.
The recordings are entered by him right into a cellphone app that relays the data to a pc within the hospital.
The information is intently monitored and any warnings that sign a deterioration in his well being are flagged to supervisors who can then take motion.
Identifying sufferers like Richard who profit from care at residence eases stress on the hospital.
It is a method developed through the pandemic and varieties a key plank of the care-at-home measures that senior well being leaders are pushing as a part of their winter disaster plans.
Read extra
NHS ready record hits document excessive of seven.2 million folks
Ambulances will go to ‘life-threatening’ calls throughout strikes
The scarcity of beds places stress on each a part of the hospital together with its emergency division. If beds can’t be discovered then ambulances can not hand over sick sufferers.
In the hospital’s new minor accidents unit Dr Ed Hartley, its medical director for emergency drugs, factors to some graphs displayed on an iPad-sized monitor mounted to the wall.
He explains there are 4 ambulances ready on the hospital able to discharge sufferers and attend the subsequent emergency, however can not as there’s nowhere to place them.
I had been advised earlier by the hospital’s chief medical officer Professor Kiran Patel that 56 sufferers had been admitted throughout the hospital and have been ready for beds.
Click to subscribe to the Sky News Daily wherever you get your podcasts
This hospital, like many throughout England, has too many sufferers which can be able to go residence however can’t be discharged as a result of there is no such thing as a social care package deal in place for them.
Dr Hartley says: “Five years ago, you wouldn’t come to emergency departments, be seen, need a bed and then wait several hours for that bed.
“That would not occur, we might have thought of that to be unacceptable. And that is now a every day incidence.”
It was right here at Coventry hospital precisely two years in the past that the world’s first COVID vaccine was given to Margaret Keenan.
That vaccine modified the course of the pandemic.
That well being disaster pressured change and innovation within the NHS, just like the digital ward that may now let Richard go residence early.
The well being service will want extra of the identical if it is to deal with the winter that’s nicely on the way in which.
Source: information.sky.com”