In the 24 years Linda Tovey has labored for the NHS, she has by no means seen the well being service so in need of workers.
“You’re just not doing the job you signed up for – it’s not possible,” the 49-year-old vital care nurse informed Sky News.
For the final two years, nurses like Linda have been leaving the well being service in file numbers, partly because of the pressures of manning a healthcare system with 133,000 vacant posts. Those that stay are left to select up the slack.
“You can’t do anything the way you’d want to do it,” Linda says. “It’s difficult to say for sure, but there are probably more errors. The idea that it’s less safe for patients causes a huge amount of stress.”
Data from NHS Digital exhibits that 15,000 nurses resigned from the well being service within the yr to March 2022, with 4,000 citing work-life steadiness as their purpose for leaving.
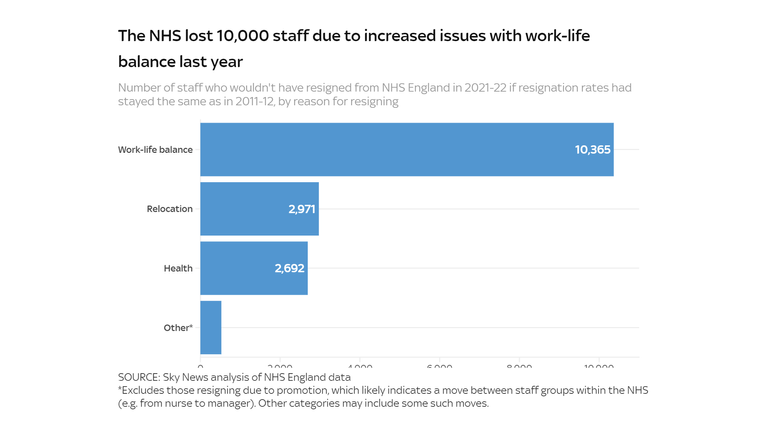
It’s not simply nurses – workers throughout the NHS are actually thrice extra more likely to give up resulting from problems with work-life steadiness than they have been a decade in the past, complicating the well being service’s efforts to plug vacancies, increase capability and convey down ready lists.
Analysis by Sky News exhibits that this enhance in resignations resulting from work-life steadiness value the NHS 10,000 workers final yr. That determine contains 203 docs, 2,800 nurses and greater than 4,100 help workers.
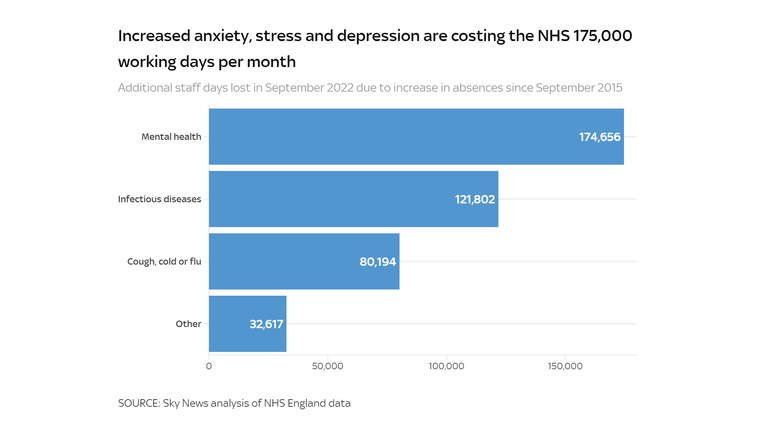
The pressure on NHS workers can also be evident within the rising quantity taking break day for psychological well being causes. In September 2022, practically half one million working days have been misplaced to nervousness, stress, or depression-related absences. That’s equal to at least one in each 80 working days, a 56% enhance since 2015.
Had charges of psychological health-related absence not elevated since 2015, Sky News evaluation has discovered, the NHS would have had a further 175,000 working days in September.
On any given day that month, one in each 42 ambulance help workers have been absent for psychological well being causes, together with one in each 52 midwives.
For docs of their second basis yr, their first yr with a full licence to apply, psychological well being absences have greater than tripled since 2015.
One NHS employee feeling the pressure is Kafeelat Adekunle, a 57-year-old neighborhood matron.
“If we had enough nurses and they were paid well, no one would be getting stretched or broken,” she mentioned. “People wouldn’t be falling sick all the time and leaving the profession.”
A current report by the Institute for Fiscal Studies discovered that nurses and midwives who took a minimum of three days off for psychological well being have been 27% extra more likely to have left the NHS altogether three months later. For consultants, the determine was 58%.
It’s not simply burnout that is inflicting workers to depart. Sky News discovered {that a} rise in relocation-related resignations value the NHS practically 3,000 workers final yr.
We don’t know precisely the place these workers are relocating to, however knowledge from the General Medical Council (GMC) means that many docs are transferring abroad.
Last yr, the GMC issued 6,950 certificates of the sort sometimes requested by docs trying to transfer overseas. Data from earlier years means that round half of those docs are more likely to stop practising within the UK inside 9 years.
“There’s definitely been a movement of EU nurses back to the EU,” says Linda Tovey.
“And other international nurses are going to places where the cost of living crisis doesn’t seem as great. People get paid more in America and Australia.”
A decade of real-terms pay cuts
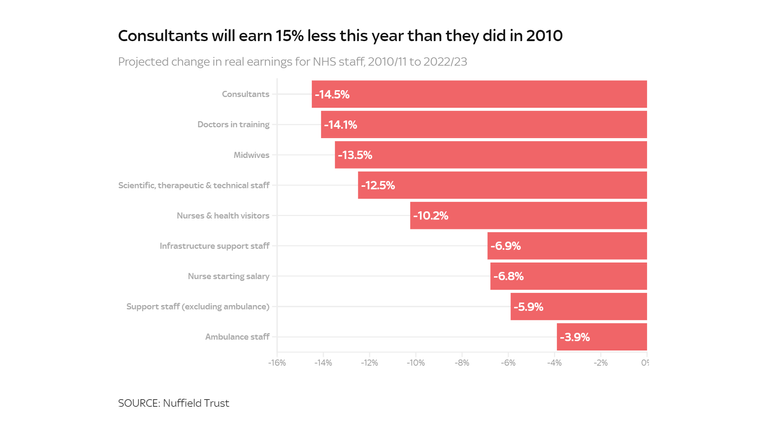
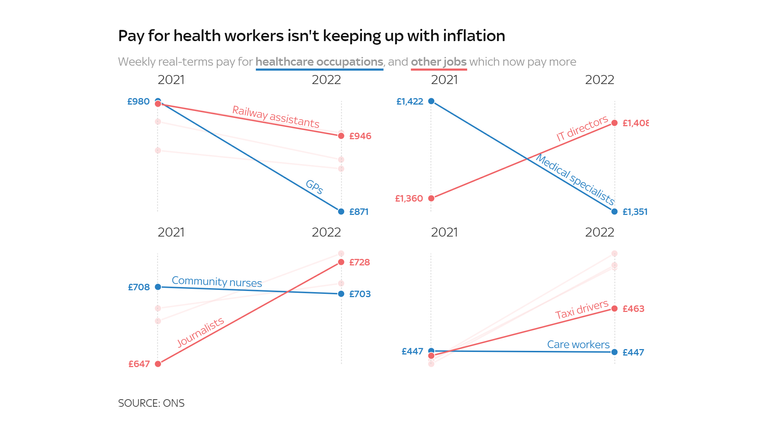
Without a rise in wages, nurses shall be paid 10% much less in actual phrases this yr than they have been in 2010, and consultants 15% much less.
“It’s not that doctors in this country are particularly poorly paid compared to other workers,” says Billy Palmer, an professional in NHS workforce points on the Nuffield Trust, a suppose tank.
“It’s that compared to some high-profile English-speaking countries we lose out. So, it could be quite tempting to go to the US or Australia because you could earn significantly more.”
In 2010, a UK medical specialist transferring to South Korea would sometimes see their earnings fall (by way of buying energy) by round 5%, in keeping with OECD knowledge. As of 2020, in contrast, they will anticipate a pay rise of 25%.
Similarly, a nurse transferring to Iceland would beforehand have taken a 13% pay reduce, however is now more likely to see a 43% bump to their wage.
Kafeelat Adekunle is among the many NHS nurses contemplating a change of surroundings.
“I’m a fighter,” she laughs, “but if anything comes up tomorrow I’m ready to go. I have a lot of family in America, and I know I could get more, even double, if I was there today.”
The identical dynamic is more likely to play into overseas healthcare employees’ choices about relocating to the UK. In 2010, a nurse coming to the UK from Slovenia may anticipate a 37% enhance to their dwelling requirements. As of 2020, they’d earn 4% extra by staying put.
“The international nurses – their expectations are always very high,” says Kafeelat. “They’ve given all their savings to escape but now they’re earning less, comparably, because of what they have to spend here. It’s a shock.
“One nurse I do know has already gone again to Nigeria – she couldn’t cope anymore. I believe it was an enormous shock for her, as a result of she thought she would earn to save lots of. But on this nation, you realize, you earn to pay your payments.”
Fewer EU staff are coming to the UK
A recent study by the Nuffield Trust found that the number of European health workers moving to the UK has declined steeply since the 2016 Brexit referendum.
Martha McCarey, one of the report’s authors, says both pay and a tightening of immigration rules for EU staff are likely to have played a role.
“There’s plenty of causes folks would need to come to the UK – they may be paid higher right here than elsewhere, or they’re supplied with the coaching alternatives they could not have at residence. With the present state of affairs, getting higher working situations or pay right here may be a much less real looking prospect.”
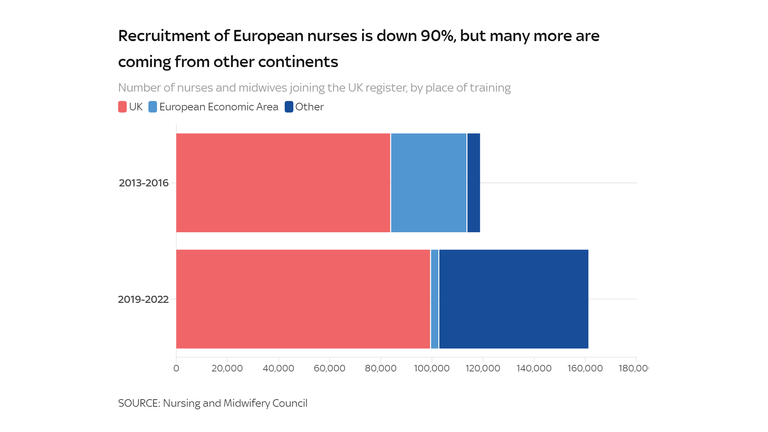
The UK recruited 27,000 fewer European nurses during the last four years than it did during the four years before the 2016 Brexit referendum.
Recruitment for nurses from other countries has increased by 53,000 – more than making up the difference.
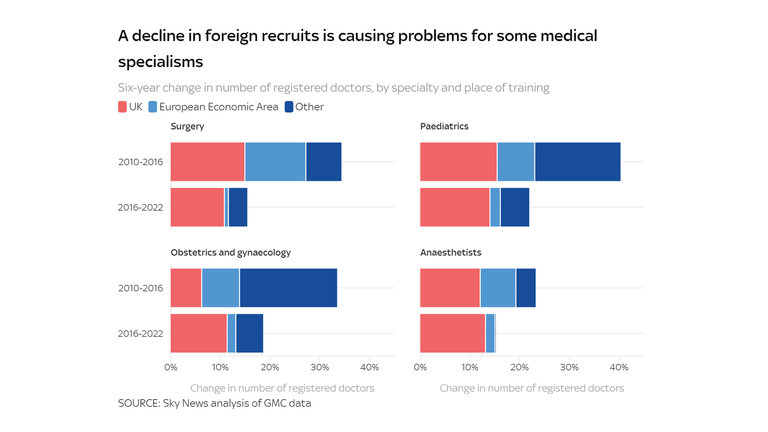
For specific sorts of physician, nonetheless, that surge in non-European recruitment by no means occurred.
In the six years earlier than the EU referendum, as an illustration, the variety of registered surgeons from exterior the European Economic Area (EEA) rose by 861. In the six years since, it has risen by simply 726. Combined with a lower in home recruits, that has meant a halving of the expansion within the variety of surgeons.
The UK depends way more on overseas recruits to workers its well being service than different international locations. As of 2020, a 3rd of docs within the UK have been skilled overseas (32%) – greater than double the OECD common of 13%. For nurses the UK is much more of an outlier, sourcing 18% of its workers from overseas in comparison with a world common of lower than 4%.
The UK’s reliance on overseas workers is rising. In 2021, for the primary time, docs from exterior the UK or Europe made up the vast majority of new additions to the medical register.
This may turn out to be extra of a difficulty over the approaching years, says Martha McCarey, as worldwide competitors for docs and nurses will increase.
The World Health Organisation estimates that there shall be a world scarcity of 18 million healthcare employees by 2030.
The UK’s dependence on overseas workers can also be doubtlessly one purpose behind the NHS’s retention points.
A current report by the Institute for Fiscal Studies discovered that, in comparison with these skilled within the UK, EU-trained consultants have been 23% extra more likely to depart the acute sector in any given month. For these from exterior the EU, the distinction was 56%.
Growing competitors with the non-public sector
It’s not simply different international locations that the NHS is competing with for workers, however different sectors inside the UK.
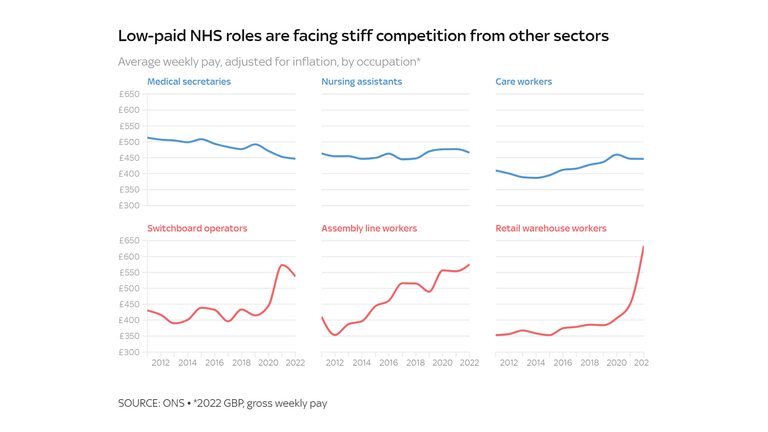
Across the NHS, wages have fallen by 4.6% in actual phrases since 2010, in keeping with the Nuffield Trust, in comparison with a 0.6% rise within the non-public sector. That has put the NHS in direct competitors with non-public employers, notably for low-paid employees.
It now pays considerably extra to be a switchboard operator, meeting line employee or warehouse worker than it does to be a medical secretary, nursing assistant or care employee.
That hole has widened within the final two years, as private-sector employers raised wages to fight their very own labour shortages.
Even higher-paying roles, like GPs and specialists, are actually dealing with elevated competitors from the non-public sector.
“The feedback you get from junior doctors is that it’s pretty toxic working in the NHS at the moment,” says Billy Palmer of the Nuffield Trust.
“Feeling valued is important, and a key way people feel valued is through pay. It’s not surprising that people are looking at what other career routes they’ve got.”
A “leaky” recruitment pipeline
The authorities has responded to workforce shortages partly by increasing the variety of medical college locations, with 4 new medical faculties created between 2019 and 2020.
The enhance in medical college students has not, nonetheless, been matched by the same enhance in coaching posts, making it tougher and tougher for trainee docs to progress.
In 2018, as an illustration, there have been 22,400 purposes for 12,400 specialist coaching posts. By 2022, a rise within the variety of medical college students meant that the variety of purposes ballooned to 36,600. The variety of posts obtainable, nonetheless, shrank to only 12,100. As a consequence, two in each three purposes have been rejected (67%) – up from lower than half (48%) in 2018.
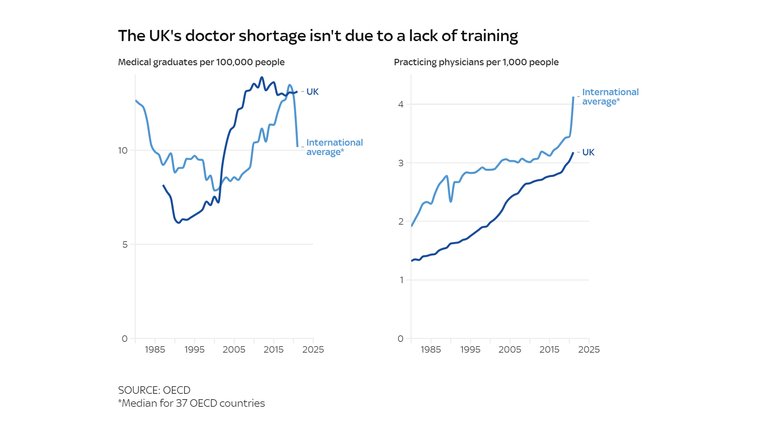
The UK has lengthy struggled to reap the benefits of its comparatively massive provide of medical college students. For virtually the entire final 20 years the UK has produced extra medical graduates than the common OECD nation. Yet for all that point, it has additionally had comparatively few practising docs.
“We’ve got a leaky pipe,” says Billy Palmer. “It’s not necessarily that we’re not training enough – there’s something happening in that domestic pipeline.”
Those points with profession development, mixed with points round pay and dealing situations, are making it troublesome for the NHS to retain workers. That, in flip, is hampering the well being service’s efforts to satisfy its bold recruitment targets.
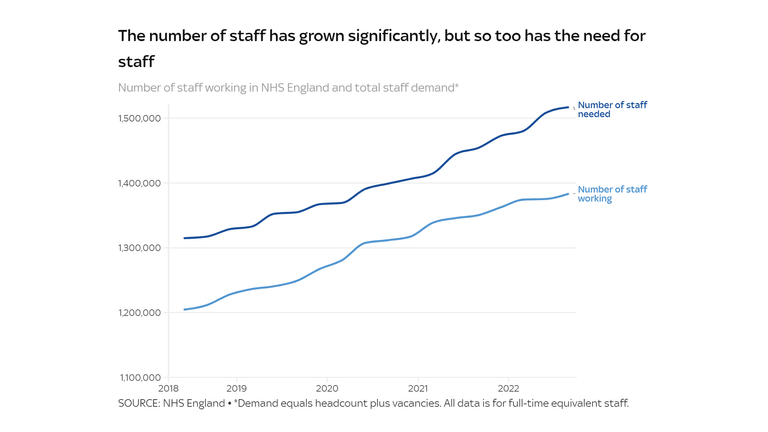
The well being service has expanded its workforce by 179,000 within the final 4 years, however rising demand for workers implies that vacancies are rising, not falling.
Billy Palmer says that the NHS has been making an attempt to increase its workforce quickly with a view to enhance capability and scale back ready lists.
“It’s partly about the amount of activity they’ve got to get through. They’ve got a pretty eye-watering backlog facing them.
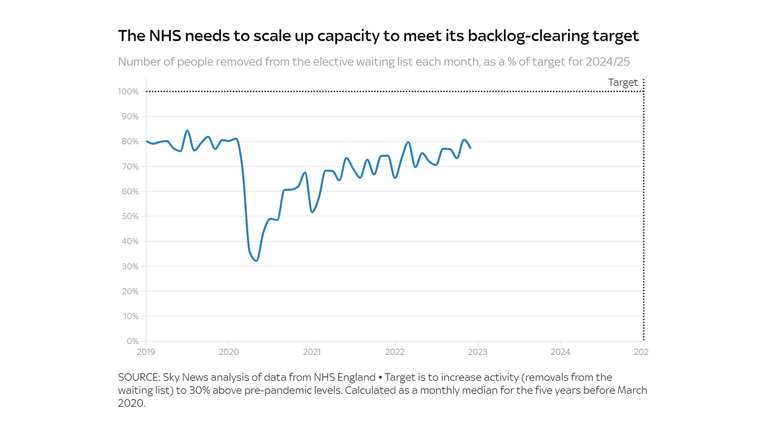
“There’s ambitions to get ranges of output to 30% above pre-pandemic ranges. Well, how do you go about attending to that? You most likely want one thing like 30% extra workers obtainable.”
The NHS remains far from meeting that target, and is only just now returning to pre-pandemic levels of elective activity.
Meeting the goal is more likely to require much more hiring over the approaching years. That’s more likely to require extra funding, however cash isn’t the one impediment.
“You’ve got capacity constraints all along the recruitment path,” Billy Palmer says.
“In the education system you need to have classrooms, supervisors, lecturers, accommodation. You also need to have placements in the services. If you’ve got staff in hospitals working flat out, it’s difficult to get them to scale up training.”
For skilled nurses like Linda Tovey, greater turnover means extra time dedicated to coaching new recruits, including to the stresses which were inflicting the retention disaster within the first place.
“It’s a real strain – you never get a day when someone isn’t following you around. And meanwhile there’s the increasing pressure to carry on, to increase productivity and get everyone through the system.”
Strikes really feel like “the only way to be heard”
Disputes over pay and dealing situations have led to a historic winter of commercial motion by NHS workers, together with the first-ever strike by the Royal College of Nursing.
Data from NHS England exhibits that the strikes have resulted within the cancellation of 92,000 appointments since December.
Earlier this month, practically 50,000 appointments have been cancelled in simply two days as nurses staged two 12-hour walkouts. The Royal College of Nursing is now making ready to stage its first-ever 48-hour walk-out, from 1 to three March.
Kafeelat Adekunle says she joined her native nurses’ strike committee as a result of industrial motion appears like “the only way to be heard.”
“It’s not just the pay, it’s the conditions in which we’re working. The government needs to come and shadow some of us. They don’t know what’s happening. They don’t know what we’re going through.
“It’s heartbreaking seeing my career taking place the drain. I’ve been a nurse perpetually and I need to be that till I retire.
“We need to do our job, we need to do it proper. We need to see our sufferers, we need to see them properly. We need to care for them. But everyone seems to be exhausted.”
The Data and Forensics workforce is a multi-skilled unit devoted to offering clear journalism from Sky News. We collect, analyse and visualise knowledge to inform data-driven tales. We mix conventional reporting abilities with superior evaluation of satellite tv for pc pictures, social media and different open supply info. Through multimedia storytelling we goal to higher clarify the world whereas additionally exhibiting how our journalism is completed.
Why knowledge journalism issues to Sky News
Source: information.sky.com”