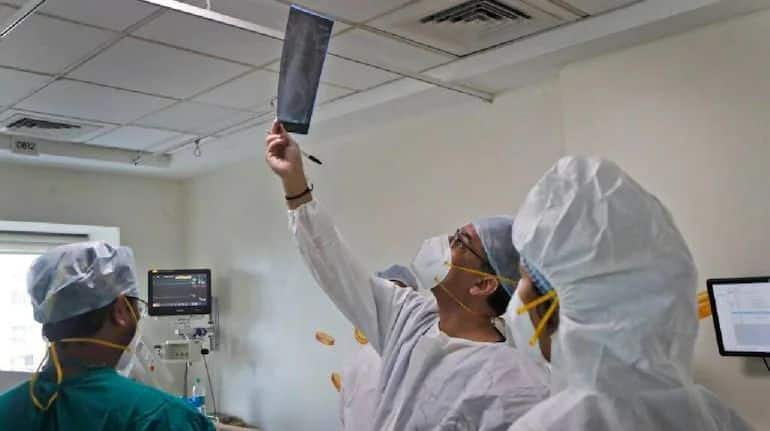
Like lakhs of Mumbaikars, 51-year-old entrepreneur Sukesh Jain (name changed) also succumbed to the corona infection earlier this month along with his wife and daughter. While his wife and daughter recovered in a few days at home, Jain decided to get admitted to a hospital as he was a sugar patient. He was discharged after three days of hospitalization, but his health insurance company rejected his cashless claim on the grounds that he had mild symptoms of corona and his condition was unfit for hospitalization.
His financial advisor told Moneycontrol, “Sukesh Jain had mild fever and cough. Although he had several pre-existing ailments as well, doctors after evaluating his condition advised Jain to be admitted to the hospital. He was treated. He was also given Remdesivir (which is possible only in the hospital). Still, the insurance company rejected his cashless claim.” Sukesh Jain complained to the regulator regarding this and at present the grievance redressal process is going on in this matter.
Treatment of patients with mild symptoms of corona
Moneycontrol had also highlighted some cases last year where insurance companies rejected claims of corona patients on the ground that their condition was unfit for hospitalisation. Some of these claims were paid when the aggrieved policyholders approached the Insurance Ombudsman.
Rishabh Pant, founder of financial planning company NRP Capitals said, “The insurance company cannot decide when the patient is to be admitted and when not. Rather, doctors and hospitals have to decide. Whether he/she needs to be hospitalized or not. Generally one would prefer to get treatment at home rather than hospitalization if given an option. In this case, insurance companies should give benefit of doubt to the patients. We have seen that generally But the settlement process of corporate group health claim is simpler as compared to claim settlement of retail policy.”
What is ICMR’s guideline for patients with mild symptoms?
The increase in the number of cases of Omicron variants may increase the number of such cases as most of the Omicron infected people are showing only mild or moderate symptoms. According to the new protocol for the treatment of corona by the Indian Council of Medical Research (ICMR), if someone has a respiratory tract infection with fever, but he is not having any difficulty in breathing or his oxygen level is low. If not, then he will be considered a patient with mild symptoms. Such COVID patients are advised to be treated at home.
Paytm’s stock hits all-time low, know if this is the right time to buy
Atul Sahai, Chairman and Managing Director, New India Assurance, the country’s largest general insurance company, said, “Preliminary data shows that the number of claims for hospitalization patients is less as compared to the second wave. The patients are recovering at home. However, there are some people who panic and got admitted to the hospitals. We are concerned about it, but we have not rejected their claim.”
Will the claim of corona patients with mild symptoms not be settled?
Atul Sahai says that the decision of the company is based on the advice of the treating doctors and the treatment protocol made by ICMR. He said, “Generously the elderly, those suffering from any other disease and those who have not received the full dose of the vaccine are more vulnerable to infection and they need to be admitted to hospitals. In such a situation, the end of the hospitals. I have to decide which patients they are admitting and who are not. We understand that many hospitals are not admitting COVID patients with generally mild symptoms.”
Insurance companies say that they are following the guidelines issued by ICMR. Bhabatosh Mishra, Director (Underwriting, Product and Claims), Niva Bupa Health Insurance said, “The ICMR protocol regarding corona treatment clearly states when a patient should be treated at home, when he should be admitted to the hospital. When should he be moved to an oxygen-equipped bed and when should he be admitted to the ICU. As an insurance company, we follow this laid down protocol. In the corona pandemic we have seen how hospitals rush when the wave intensifies. There is a shortage of beds. Patients who can be treated at home if they are also admitted, then patients who require hospitalization will not get beds in time. Hence, in such cases In cases where mild symptomatic patients that did not require hospitalization were still admitted by mistake, we unfortunately could not pay their claims.”
Sania Mirza Retirement: ‘2022 Will Be My Last Season’, Sania Mirza Announces Retirement From Tennis
How do insurance companies reject claims?
Some insurance broking and management firms also confirm that in case of mild symptomatic patients being hospitalized, insurance companies are rejecting their claims. Anuj Jindal, Founder, Sureclaim.in said, “One of the reasons for claim rejection is that some patients get admitted to hospitals on the apprehension that their condition may turn critical later. In such cases, we have observed that if If the situation is not critical at the time of admission and remains the same throughout, some insurance companies reject the claim.”
After the claim is filed, the insurance companies also conduct their own investigation and if the patient’s condition does not match with the condition stated in the hospital, then their claims are rejected. Kulin Shah, co-founder and COO of Onsurity, a health-tech firm, said, “The team of doctors on behalf of insurance companies, based on the clinical documents of the patient and the recommendations given by the doctors, decides whether he needs to be admitted to the hospital. required or not.”
This is the last resort for policyholders
If the insurance company has rejected your health claim and if you believe that your hospitalization was justified, then you do not have to accept the decision of the insurance company as final. In such a situation, you can first register your complaint with the grievance redressal department of the insurance company. If your complaint is not resolved satisfactorily here, then you should approach the Insurance Ombudsman located in your city. Here too, if nothing happens, you can approach the Consumer Court, which is the last resort in all such cases.
.

